Osteoporosis, or thinning of the bones, occurs with hormonal deficiency, lack of exercise, weight loss, cigarette smoking, alcohol use, steroid therapy, high protein diets and vitamin D deficiency. Certain medications increase bone loss, including cortisone-like drugs and antidepressants.
Fractures due to osteoporosis occur most often in the hip or lower back, can be very painful and cause permanent loss of mobility. In older people, hip fractures can often lead to mortality. Osteoporosis is more common in tall, light-complexioned women. However, a quarter of hip fractures occur in men, and as men live longer, the number who suffer a hip fracture due to osteoporosis is steadily rising. More than half of fractures due to bone loss occur in people whose bones are thinning but aren’t quite thin enough to be labeled osteoporosis. They’re in a gray zone known as osteopenia.
Osteoporosis – Treatment and Prevention
The best natural treatments for both osteoporosis and osteopenia are also good for prevention.
1. Calcium and magnesium are required to build healthy bone matrix. Both calcium and magnesium help to slow bone loss when increased levels are circulating in the blood.
2. Vitamin D is a fat soluble vitamin that is generated in the skin when it is exposed to sunlight. Vitamin D is required for absorption of calcium in the gut. Vitamin D is proven to support healthy bone density. Many researchers point to an unrecognized epidemic of vitamin D deficiency among older Americans, suggesting that of those 200,000+ persons who suffer hip fractures each year, many are vitamin D deficient.
3. Strontium is a naturally occurring mineral, and is naturally found in the human body. Strontium has an affinity for bone and is taken up at the bone matrix crystal surface. The influence of strontium on bone metabolism has been researched since the 1950’s. Studies show that strontium positively affects bone metabolism to promote bone formation and decrease bone resorption, and can actually increase bone density. Researchers reporting in the New England Journal of Medicine found a 41% reduction in vertebral fractures over 3 years when adding strontium to a stable calcium and vitamin D diet regimen.
4. Vitamin K is a fat soluble vitamin available in several forms. Vitamin K is required for the synthesis of osteocalcin, a bone protein integral for bone formation. Osteocalcin provides the structure and order to bone tissue; without it, bones would be fragile and easily broken. In humans, vitamin K levels fall during recovery from a fracture evidencing that this nutrient is actually drawn from the rest of the body to the site of the fracture. Vitamin K2 is found in meats and dairy products and is produced naturally by bacteria. Its more popular cousin, vitamin K1, is found in greater concentrations in green leafy vegetables. Both forms are used to maintain a more healthy bone matrix, but vitamin K2 has a longer half-life in the body.
5. Hormone replacement therapy to include natural estrogen and testosterone, DHEA and occasionally growth hormone. Hormone pellets have shown the greatest protection for patients at risk for osteoporosis, or those who have it.
6. Weight-bearing exercise, at least 30 minutes every day has been shown to promote healthy bone structure and prevent osteoporosis.
7. Drink green tea, or supplement with green tea extract. A study published in the American Journal of Clinical Nutrition shows elderly women who drank tea had higher bone density in their hips and less bone loss than women who didn’t drink tea. Researchers say the results confirm previous studies that have suggested drinking tea may protect against bone loss and osteoporosis.
8. Prescription pharmaceuticals when osteoporosis is severe, when the above measures cannot be employed, or when bone density declines despite these therapies. It is unusual for pharmaceuticals to be needed when intervention occurs early.
In the U.S. alone, some 10 million people have osteoporosis and 34 million are estimated to have osteopenia. With the population rapidly aging, the government estimates half of Americans over 50 will be at risk of fractures from too-thin bones by 2020.
The World Health Organization funded a Web-based tool called FRAX, unveiled last week, that helps calculate the odds of a hip, wrist, shoulder or spine fracture within the next 10 years for anyone 40 or older in nine different countries – regardless of whether they have full-fledged osteoporosis or just low bone mass. (CLICK HERE to use the FRAX calculation tool online – you will need data from a current DXA bone densitometry test to do this calculation. To start, choose your nationality under the calculation tool section at the top of the page.)
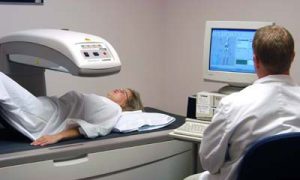
Patient Receiving a DXA Scan
Most women and many men are at risk for osteoporotic bone fractures as they get older. At the Institute for Progressive Medicine, we have great success in preventing and reversing osteoporosis.
A DXA bone density study is the easiest and most accurate way to evaluate for osteoporosis. The test is performed in our office, takes only minutes and involves negligible x-ray exposure, approximately 100 times less than a chest x-ray. The test should be performed in any woman approaching menopause, since menopause is the time of greatest bone loss. Other risks for osteoporosis in both men and women include limited movement sue to paralysis, steroid therapy, malnutrition, scoliosis, back pain or after any fracture. Additionally, men should have a DXA scan if they are receiving prostate cancer therapy. We also routinely test for vitamin D levels, since the majority of men and women are deficient.